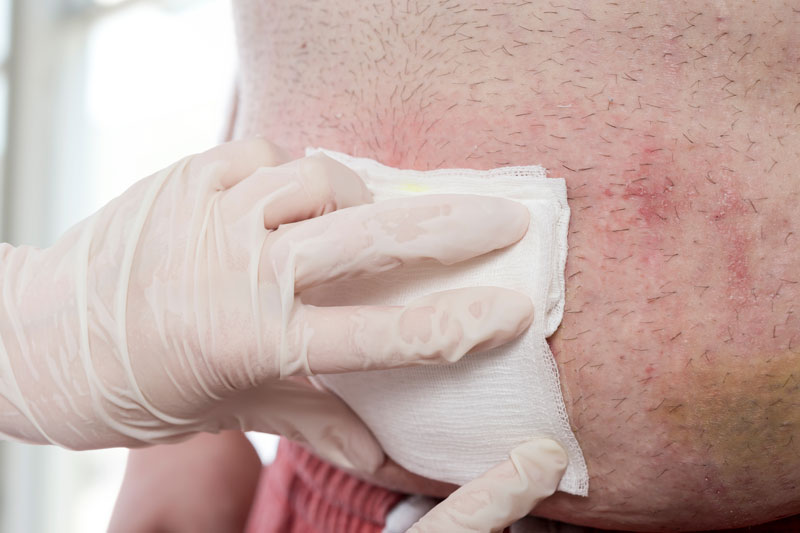
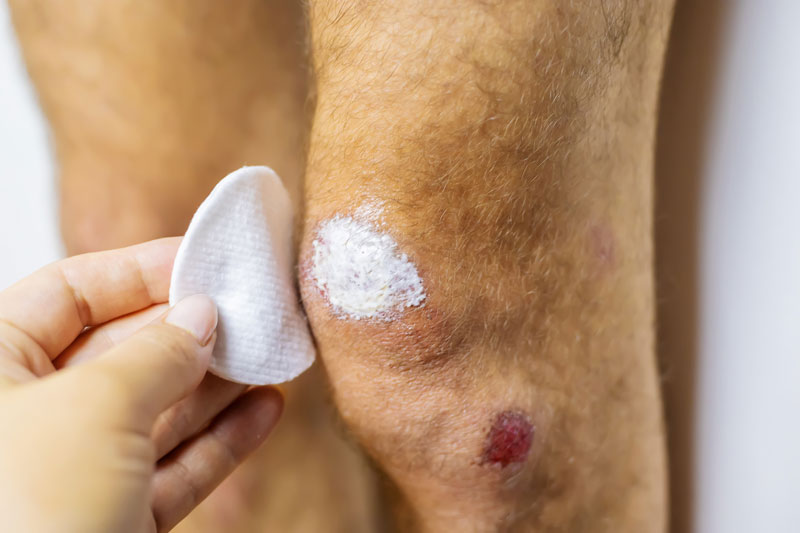
What are Pressure Ulcers?
What Causes pressure Ulcers?
Symptoms of Pressure Ulcers
Pressure ulcers can manifest in varying degrees of severity, with symptoms that may include redness or discoloration of the skin, tenderness, and warmth in the affected area. As the condition progresses, the skin may develop open sores, blisters, or shallow wounds. In some cases, pressure ulcers can extend to deeper tissues, leading to the formation of a cavity or a visible, exposed wound. Patients may experience localized pain, itching, or a burning sensation around the affected site. If you or a loved one experience any signs of pressure ulcers, do not hesitate to seek expert wound care services for comprehensive evaluation and treatment.
Treatment Options for Pressure Ulcers
When it comes to pressure ulcers, early and comprehensive treatment is crucial for effective healing and preventing further complications. At Mobile Wounds, our affiliated practices offer a range of specialized treatment options tailored to each patient’s unique needs. Our team of experienced wound care professionals is dedicated to delivering compassionate and evidence-based care to promote optimal recovery. Treatment options for pressure ulcers may include:
- Wound Dressings: Applying appropriate dressings to protect the ulcer and promote a moist wound-healing environment.
- Debridement: Removing dead or damaged tissue to facilitate the healing process.
- Offloading: Relieving pressure on the affected area through repositioning or the use of specialized cushions or mattresses.
- Negative Pressure Wound Therapy (NPWT): Applying controlled suction to the wound to encourage healing and reduce infection risk.
- Topical Medications: Using creams, ointments, or gels to promote healing and manage infection.
- Pain Management: Addressing discomfort associated with pressure ulcers through various methods.
- Nutritional Support: Ensuring adequate intake of essential nutrients to support the healing process.
- Education and Prevention: Offering guidance on proper wound care at home and preventative measures to avoid future ulcers.
- Advanced Wound Healing Modalities: Employing growth factors, cellular therapies, or skin substitutes to enhance healing in complex cases.
Trust Mobile Wounds and our network of leading wound care providers to deliver exceptional care and support throughout your pressure ulcer healing journey.
Frequently Asked Questions about Pressure Ulcers
1. What are the risk factors for developing pressure ulcers?
Several factors can increase the risk of developing pressure ulcers. The most common risk factors include:
- Immobility: Being bedridden or confined to a wheelchair for extended periods reduces the ability to shift positions and relieve pressure on vulnerable areas.
- Lack of Sensation: Conditions such as spinal cord injuries or neurological disorders may result in reduced sensation, making it challenging to detect discomfort or pressure on the skin.
- Poor Nutrition: Inadequate intake of essential nutrients can compromise the skin’s integrity and hinder the body’s ability to repair and regenerate tissues.
- Age: Elderly individuals are more susceptible to pressure ulcers due to changes in skin elasticity and reduced mobility.
- Medical Conditions: Chronic illnesses, such as diabetes, vascular disease, or malnutrition, can increase the risk of developing pressure ulcers.
- Incontinence: Prolonged exposure to moisture can weaken the skin, making it more susceptible to damage and ulcer formation.
2. How can pressure ulcers be prevented?
Preventing pressure ulcers is crucial, especially for individuals at higher risk. Some effective prevention strategies include:
- Regular Repositioning: Changing positions frequently is essential to relieve pressure on vulnerable areas. Bedridden patients should be repositioned every two hours, while wheelchair-bound individuals should shift their weight at least every hour.
- Specialized Support Surfaces: Using pressure-reducing cushions, mattresses, or overlays can help distribute pressure more evenly and minimize the risk of ulcers.
- Skin Care: Keeping the skin clean, dry, and moisturized can help maintain its integrity and reduce friction-related injuries.
- Nutrition: A well-balanced diet rich in protein, vitamins, and minerals is essential for supporting healthy skin and promoting tissue repair.
- Regular Assessment: Routine skin inspections can help identify early signs of pressure ulcers, allowing for timely intervention and treatment.
- Mobility and Exercise: Encouraging regular physical activity, within the individual’s capabilities, can enhance blood circulation and reduce the risk of ulcers.